Estimated reading time: 10 minutes
One of the things that we’re just starting to hear more about is “long COVID” or “post-COVID conditions. I saw an article on the American Management Association (AMA) website estimating at 10%-30% of patients might experience long COVID after recovering, even if they don’t think they were very sick in the first place.
Post-COVID symptoms can include breathing problems, extreme fatigue, and cognitive and memory issues. And according to the latest research, these symptoms can last up to a year. In an article published in The New York Times, Dr. Ziyad Al-Aly, chief of research and development at the V.A. St. Louis Health Care System and a clinical epidemiologist at Washington University in St. Louis shared that this new information about long COVID “can potentially translate into millions of people with new diabetes, heart disease, kidney disease, and neurologic problems. These are lifelong conditions — certainly manageable, but not curable conditions.”
While the news might be reporting that the pandemic phase of COVID is behind us, for some people, they’re stilling dealing with the symptoms. It’s possible that an employee who had COVID might ask for their work to be modified in some way.
I’m not aware of any specific legislation that protects individuals who have long COVID, but there are laws in place that protect employees when they are sick, recovering, or need accommodation. So, employers need to think about these scenarios now because that way, they have some process in place.
Which is exactly why I asked my friend and labor attorney Carrie Cherveny to join us for a conversation about long COVID and what employers should know. Carrie is senior vice president of strategic client solutions in HUB International’s risk services division. In her role, she works with clients to develop strategies that ensure compliance and risk mitigation when it comes to insurances such as health and welfare programs and employment practices liability. Carrie has been helping us throughout the pandemic to understand the matters that organizations need to consider.
And while Carrie is a lawyer, please don’t forget that her comments shouldn’t be construed as legal advice or as pertaining to any specific factual situations. If you have detailed COVID questions, they should be addressed directly with your friendly neighborhood labor and employment attorney.
Carrie, thanks for helping us with this topic. Let’s get right to the matter. Does long COVID meet the description of a “serious health condition” under the Family and Medical Leave Act (FMLA)?
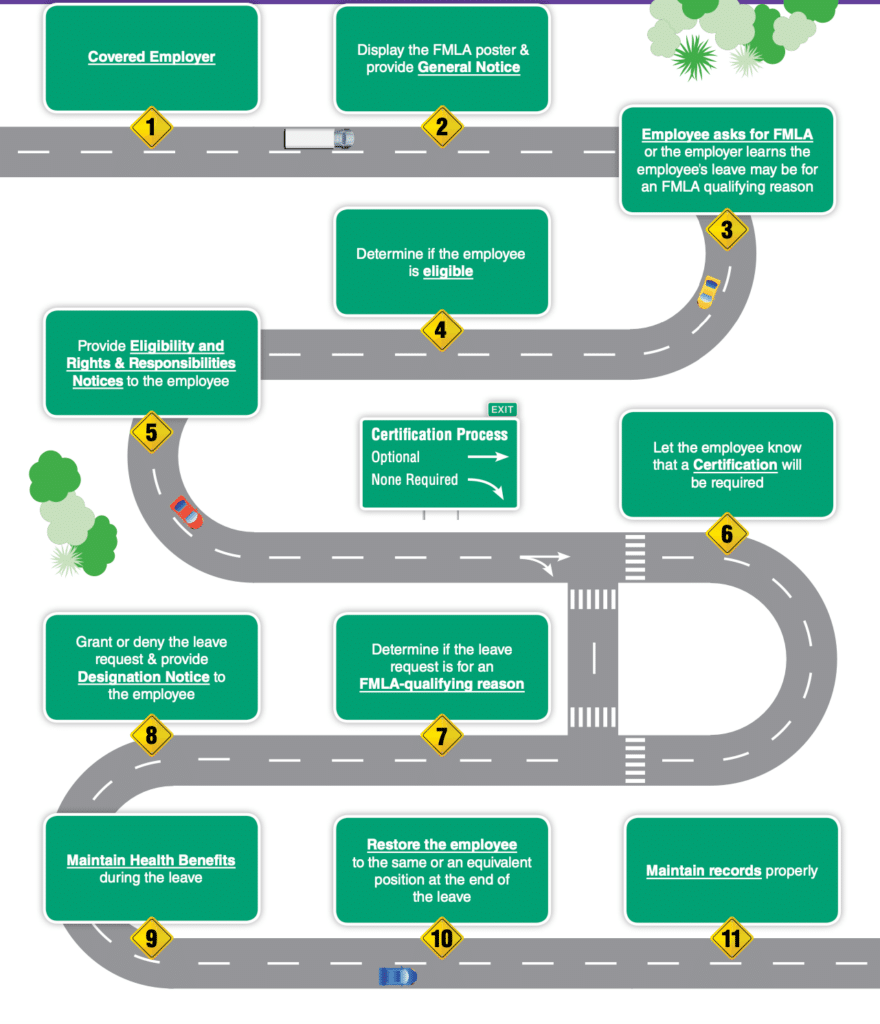
[Cherveny] It depends. Employers must remember the foundational requirements of the FMLA. The employer must go through the FMLA process when an employee experiences a condition that impacts their ability to work (whether on a consistent or intermittent basis). This means that the employer should follow the Department of Labor’s (DOL) FMLA roadmap. This includes:
(1) informing the employee of his/her eligibility for FMLA;
(2) assessing the employee’s health condition from the lens of the FMLA; and
(3) making an FMLA determination.
We always recommend employers utilize the certification forms provided by the DOL. For example, an employee experiencing long-term symptoms of COVID may require regular breathing treatments and physical therapy necessitating intermittent FMLA. Under these circumstances, the employer should provide the employee with the Notice of Eligibility & Rights and Responsibilities along with Certification of Health Care Provider for Employee’s Serious Health Condition. In more serious cases, an employee may be required to spend the night in the hospital.
Likewise, an employee may be providing care for an immediate family member with long-haul COVID and may be eligible for FMLA to provide that care. In the case of a family member, the employer would provide the same eligibility form but instead include the Certification of Health Care Provider for Family Member’s Serious Health. What’s important here is that the employer follows FMLA steps to arrive at a determination.
You mentioned certification forms. It makes sense that if an employee brings up that they are experiencing symptoms of long COVID, an employer can request a doctor’s certification. But what about when an employee calls in sick for COVID reasons? Can the employer require a doctor’s note for them to return to work? Are there any other requests that the employer might want to consider?
[Cherveny] Employers may require a health care provider’s release to return to work but this requirement should be consistent for any employee serious health condition. In fact, the FMLA provides:
- An employer may have a uniformly-applied policy or practice that requires all similarly-situated employees who take leave for their own serious health condition to obtain and present certification from the employee’s health care provider that the employee is able to resume work as a condition of restoring an employee.
- This fitness-for-duty certification can be requested only for the health condition that caused the employee’s need for FMLA leave. Certain limitations apply to the frequency with which an employer may require a fitness-for-duty certification for absences taken on an intermittent or reduced schedule basis.
The FMLA approach (uniform requirement for a fitness for duty) is the recommended approach for all return to work (even those that are not FMLA eligible) after an employee absence for their own injury or illness. Meaning, HR should not apply different return to work requirements for particular employees or conditions. If an employer is going to require a release for work, it should do so consistently for any employee that takes a leave of absence for their own medical condition.
Is an employee able to make a workers’ compensation claim related to long COVID?
[Cherveny] This is another ‘it depends’ answer. Under certain circumstances, claims from health care providers and first responders may be allowed. Additionally, employees’ claims may be compensable if they can provide medical documentation demonstrating that their condition falls within the scope of the individual state’s and/or policy’s definitions of illnesses. Each claim will be reviewed upon its own merits. Some of the factors that will be reviewed to determine compensability will be whether the disease is ‘arising out of’ the course and scope of employment and/or whether it contracted due to conditions peculiar to the work.
Generally, coverage is specifically aligned with state and jurisdictional guidelines. Depending on the state, ‘arising out of’ employment generally requires a causal connection between the injury and the employment, whereas ‘in the course of’ employment refers to a causal connection to the workplace and looks at the time, place, and circumstances under which the illness occurred. Across National Council on Compensation Insurance (NCCI) states, ‘course and scope’ statutes generally applies as providing compensation for personal/accidental injury arising in and out of employment and occupational disease arising in and out of employment.
Much like the FMLA and the Americans with Disabilities Act (ADA), each workers’ compensation claim will be evaluated on its own merits and subject to each individual state’s COVID-19 compensability requirements.
Speaking of the ADA, can an employee ask for an accommodation based on long COVID under the Americans with Disabilities Act (ADA)? If so, what would be an example of a reasonable accommodation?
[Cherveny] An individual experiencing more severe and/or long-lasting symptoms from COVID-19 may qualify for an accommodation under the ADA. But how can HR determine whether an employee is experiencing COVID long-hauler symptoms that interfere with their ability to perform the essential functions of the job? In other words, when does a COVID long-hauler become eligible for the rights and benefits of the Americans with Disabilities Act? To begin with, HR professionals should engage in the ADA ‘interactive process’. The interactive process is simply a cooperative and collaborative case-by-case assessment to assess the employee’s circumstances and the requirements of the ADA. In general, employer’s duty to engage in the interactive process requires:
- To do more than remain passive (simply answer specific questions by employee is not enough)
- Take initiative and clarify what accommodation is required
- Engage in a meaningful and direct conversation
- No breakdown in the process by any of the parties
- Seeking reasonable documentation to establish the need for accommodation (medical documentation may be required, limited religious inquiry may be made). An employer cannot ask for documentation when: the disability and the need for reasonable accommodation is obvious, or the individual has already provided the employer with sufficient information
- Explaining to employer why provided documentation is insufficient
- Exploring alternative accommodations when initially offered accommodation is rejected by an employee
- Spending time on the process and documenting efforts to accommodate
The limitations from COVID-19, like other disabling conditions, do not have to last any particular length of time to be substantially limiting. For example, if the individual experiences episodic symptoms (meaning they come and go) the individual may have an actual disability if it substantially limits a major life activity when active. For example, an individual diagnosed with COVID-19 who experiences ongoing and/or intermittent headaches, dizziness, ‘brain fog’, and/or breathing issues, may be substantially limited as to major bodily functions and/or major life activities. Likewise, an employee with these symptoms may not be able to perform the essential functions of their job without an accommodation. For instance, a server in a restaurant who is short of breath may not be able to work lengthy shifts or carry heavy trays. However shorter shifts and a food-runner may be an appropriate accommodation based on the employee’s facts and circumstances.
Under the ADA, employers cannot consider mitigating measures when determining whether COVID-19 substantially limits a major life activity. This means that the employer must consider the symptoms without the benefit of medications or other measures to lessen their impact on the employee.
Long-haulers may also be eligible for short and/or long-term disability insurance wage-replacement benefits. If the employee’s symptoms prevent the employee from working in either their own job or any job, disability insurance may provide some portion of wage replacement benefits for a pre-determined period of time. Much like the ADA, the disability benefits determination is made on a case-by-case basis and requires an assessment of the employee’s condition. The terms of insurance policy will dictate whether, based on the employee’s medical circumstances, benefits eligibility exists under the disability insurance program.
Last question. From personal experience, I know what it feels like to return to the workplace after an accident and have to navigate with my coworkers in terms of what I was able and unable to do. Right now, employers are trying to figure out the best way to bring employees back onsite. If an employee is returning to the worksite and they are unable to do everything they used to do, what suggestions do you have for employers about how to respectfully redistribute the work without breaking confidentiality rules?
[Cherveny] It’s important to remember that employee medical information is confidential and protected by the ADA. This means that only those who need to know may be made aware of the employee’s medical condition. The ADA construes ‘need to know’ very narrowly. Generally, HR may know employee confidential medical information, and under some circumstances, the employee’s manager or supervisor. This means that conversations with coworkers about the redistribution of duties must be limited to the duties themselves and not an employee’s underlying health condition.
Employers will have to carefully navigate the job reassignment discussion and citing neutral reasons such as business needs, organizational objectives, and cross-training opportunities. Likewise, the evolution of workforces to hybrid/remote has necessitated job assignment changes. These changing work environments provide a neutral backdrop for a job accommodation redistribution of duties without revealing confidential medical information.
Often, the employee experiencing the medical condition will share it with co-workers. Under those circumstances, the employer has not violated any privacy rules because the employee chose to share their own medical information.
I want to extend a huge thanks to Carrie for sharing her knowledge with us. If you’re looking for a resource to help your organization maneuver through the pandemic, be sure to check out the HUB International COVID-19 Resource page.
I understand that today’s article has a lot of information to unpack. It’s exactly the reason that organizations need to think about what they will do if an employee is experiencing post-COVID symptoms. Maybe some organizations are already dealing with this. While restrictions are relaxing, that doesn’t mean cases are. HR departments need good information to help the organization make the right decisions – for the business and their employees.
Image captured by Sharlyn Lauby while exploring the University of Florida in Gainesville, FL
COVID FMLA roadmap courtesy of the Department of Labor – Employers Guide to FMLA
24